Scoliosis Surgery Guide:
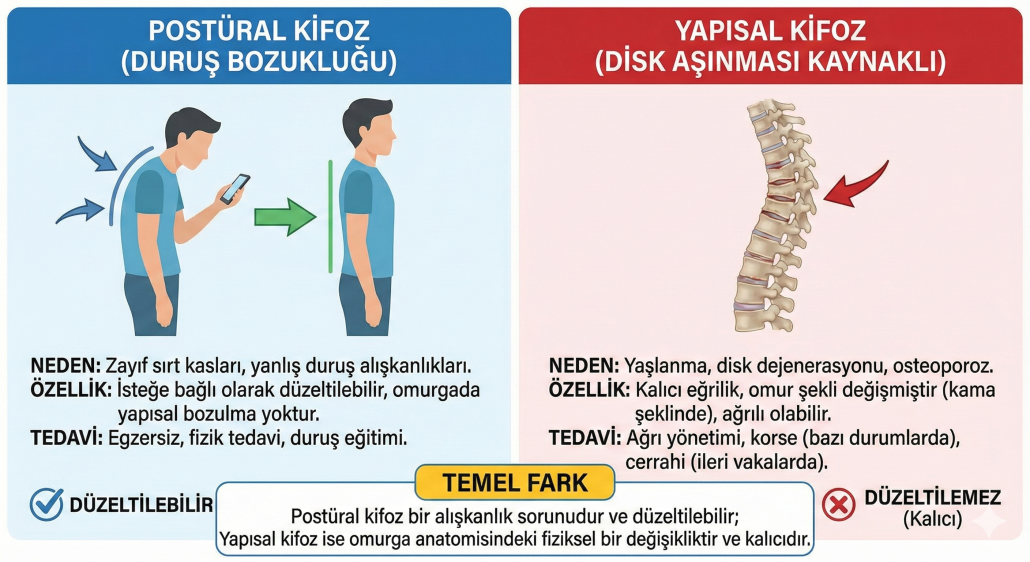
The biggest concern for many patients and families diagnosed with scoliosis (spinal curvature) is whether the treatment process will require surgical intervention. The first rule we always emphasise in our clinical practice is this: Not all cases of scoliosis require surgery. The vast majority of cases can be managed through observation, physiotherapy and the use of a brace.
However, when the curvature exceeds certain limits and continues to progress, surgical options become medically necessary to preserve spinal biomechanics and prevent potential health problems. In this article, we take an objective look at the place of scoliosis surgery in the medical literature, current surgical methods, and the recovery process.
How is the Decision Made to Undergo Scoliosis Surgery?
The decision to perform surgery is not an immediate choice; it is the result of a mathematical and clinical assessment based on the patient's age, bone development and the degree of curvature (Cobb angle).
According to the general medical approach, the main situations in which scoliosis surgery is considered are as follows:
- Degree of curvature: Situations where the Cobb angle exceeds 40-45 degrees and asymmetry becomes pronounced.
- Progress Rate: Despite corset treatment and exercises, the curvature cannot be stopped during the growth phase and continues to increase.
- Physical Effects: Risk of impaired respiratory function due to reduced chest cavity volume in cases of severe curvature (generally 70 degrees and above).
- Pain and Loss of Function in Adults: Cases of degenerative scoliosis that occur alongside nerve compression (canal narrowing) in advanced age and reduce quality of life.
Safety in the Surgical Process: Neuromonitoring
The most common fear associated with spinal surgery is the risk of nerve damage. In modern spinal surgery, devices called neuromonitors (nerve monitoring) are used as standard to minimise this risk.
This system simultaneously monitors nerve signals passing through the spinal cord during surgery. If the slightest slowdown in nerve transmission is detected during surgical manoeuvres, the system immediately alerts the surgeon. Thanks to this technology, the safety margin for scoliosis operations has reached much higher levels compared to previous years.
Post-operative Recovery and Return to Normal Life
Scoliosis surgery is a major orthopaedic procedure; however, patients' recovery times and return to daily life are faster than expected.
- Hospitalisation: Following the operation, patients typically stay in hospital for 4 to 6 days.
- Standing Up: Patients are assisted to stand and walk with the help of a physiotherapist within the first 24 hours after surgery.
- Back to School/Work: Most patients can return to desk jobs or school life 3 to 4 weeks after surgery.
- Back to Sport: While light exercise such as walking and swimming can generally be started in the first few months, a return to competitive sports that require contact or strain the spine should wait until the bone has fully healed (on average 6-12 months).
Frequently Asked Questions (FAQ)
1. How long does scoliosis surgery take? The duration of the operation varies depending on the degree of curvature, the number of vertebrae to be treated, and the surgical technique used, but it can generally be completed within 4 to 7 hours.
2. Does height increase after scoliosis surgery? Yes, height increase is a natural result of the surgery. With the straightening of the curvature in the spine (C or S shape) to a straight line, an increase in height of 2 to 6 cm is generally observed in patients, depending on the severity of the deformity.
3. Are the screws inserted during surgery removed later? Titanium screws and rods used in spinal fusion surgery are biocompatible materials. Unless there is a medical necessity, such as a very rare infection or material fatigue, they remain in the body for life; there is no need to remove them.
Legal Notice: This content is for informational purposes only. It is not a substitute for diagnosis and treatment. Consult your doctor if you have any health concerns.
Prof. Dr. Çağatay Öztürk Orthopaedic and Traumatology Specialist | Spinal Surgery